3 Ways to Make Sure Your Cancer Treatment Plan Works for You
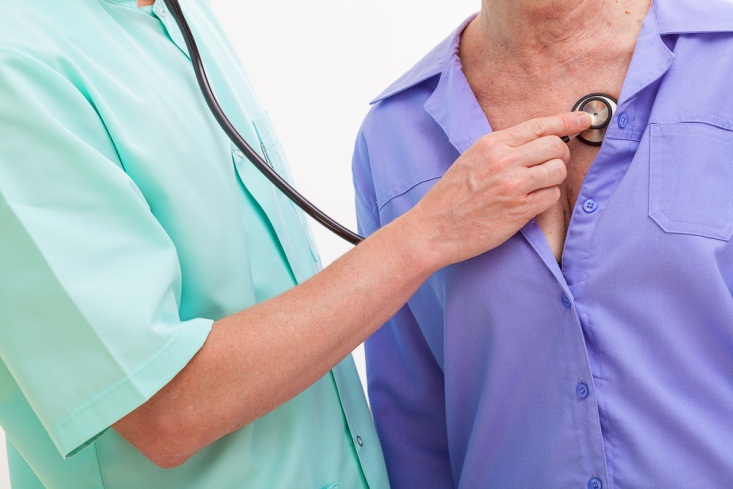
 A cancer diagnosis can be one of the most overwhelming to receive, and if you’re like many patients, you may feel rushed to make decisions about your treatment. While your doctor may want you to start looking at treatment options as soon as you receive your diagnosis, you’ll most likely have some time to think things over and decide for yourself what treatment plan will work best for you. Remember that your ultimate decision doesn’t have to be set in stone — if you change your mind about treatment midway through the process, that’s okay, too.
A cancer diagnosis can be one of the most overwhelming to receive, and if you’re like many patients, you may feel rushed to make decisions about your treatment. While your doctor may want you to start looking at treatment options as soon as you receive your diagnosis, you’ll most likely have some time to think things over and decide for yourself what treatment plan will work best for you. Remember that your ultimate decision doesn’t have to be set in stone — if you change your mind about treatment midway through the process, that’s okay, too.
1) Don’t Face the Decision-Making Process Alone
Choosing a cancer treatment center and a treatment plan is a big deal, and you need support. Your doctor can offer you the support of his or her expertise, but you can also get support from friends and loved ones. A support group or counselor can also help.
It’s okay to not want to make all of your treatment decisions — many people leave some or all of these decisions up to their treatment team or a designated friend or relative. Some people don’t even want to know details about the treatment they’re receiving or their chances of survival. Alternatively, you may want the final say on any decisions regarding your treatment.
2) Choose a Hospital or Treatment Center
Whether you ultimately go with a specialized cancer treatment center, like our cancer center in Los Angeles, or a community or academic hospital is up to you. A large, specialized cancer treatment center will give you access to many different treatment methods and cancer specialists in the same building, and will make it easier for your treatment team to collaborate. However, if you live far from such an institution, a local community or research hospital may be the best choice. Some things to consider when choosing a hospital include:
- Is this hospital convenient to my home, and if not, can I afford to travel to it?
- Will I be able to undergo clinical trials at this hospital?
- Does the hospital offer support groups for me and my family?
- Will my insurance cover treatment here?
- Does the doctor who will be in charge of my treatment have a good reputation?
Research your cancer treatment options carefully, and understand the differences in treatment approach between a cancer center and a general hospital.
3) Keep Talking to Your Doctor
Your goals for and feelings about treatment may change as treatment progresses. Most cancer treatment options cause side effects that can affect your quality of life; your doctor will be more than willing to offer palliative care to help relive these side effects.  If side effects are too severe or you have second thoughts about your treatment decision, you’re allowed to change your mind. Treatment can affect your health, career, and personal life in ways you might not expect. It’s part of your treatment team’s job to help you cope with these changes.
If side effects are too severe or you have second thoughts about your treatment decision, you’re allowed to change your mind. Treatment can affect your health, career, and personal life in ways you might not expect. It’s part of your treatment team’s job to help you cope with these changes.
While making a decision about cancer treatment can be daunting, it’s not something you should have to do alone. Friends, loved ones, and a supportive treatment team can help you make the best decision for you, and help you ensure that you’re pursuing the right options throughout your treatment.
More
5 Foods You Should Eat During Cancer Treatment
 Cancer treatments can take a harsh toll on your body, and keeping your strength up isn’t easy. Getting plenty of sleep, exercising regularly, and eating well are all important parts of taking care of yourself during cancer treatment.
Cancer treatments can take a harsh toll on your body, and keeping your strength up isn’t easy. Getting plenty of sleep, exercising regularly, and eating well are all important parts of taking care of yourself during cancer treatment.
But those things are easier said than done. Eating can be especially difficult, as cancer treatment side effects can make it hard to chew, swallow, and keep down food. When you’re going through cancer treatment, focus on eating nutritious, calorie-dense foods like some of these.
Eggs
Eggs are packed with protein, making them an excellent choice for people going through cancer treatment. One egg contains seven grams of protein, about as much as an ounce of cheese, fish, poultry, or beef. Eggs also contain selenium, a mineral that could ease the side effects of chemotherapy and boost your immune system during cancer treatment. The vitamins D and E in eggs may protect your body from some of the toxic effects of chemotherapy, and may combat feelings of numbness in the hands and feet that occur due to chemotherapy.
Plus, eggs are soft and easy to chew and swallow. That’s a bonus if you’re struggling with a sore mouth and throat due to cancer treatment.
Yogurt
Another easy-to-swallow food, yogurt, contains plenty of protein and calcium for strong bones, which is especially important for women going through treatment for reproductive cancers. Just make sure you choose live-culture yogurt, since it’s these probiotics that are largely responsible for helping you stay healthy during cancer treatment. Probiotics help prevent constipation and diarrhea by supporting an appropriate balance of intestinal flora.
Broth
It’s always important to stay hydrated, but it’s even more important to do so when you’re going through cancer treatment and experiencing side effects like vomiting and diarrhea. Whether it’s beef, chicken, or vegetable broth, the salty liquid will help keep your body’s electrolytes in balance. Even a clear miso soup will do. These foods may also contain other vitamins and minerals that can help you stay healthy.
Of course, doctors recommend consuming eight to 12 cups of liquid a day to prevent dehydration during cancer treatment, and that’s a lot of broth. Popsicles, water, pasteurized juice, and sports drinks are also good ways to say hydrated during cancer treatment.
Legumes and Beans
Legumes and beans are among the most nutritious foods you can eat during cancer treatment. They’re rich in B vitamins and protein, which your body needs for everything from cell repair to immunity and healing. Beans and legumes are also high in fiber, which can help protect you from diarrhea or constipation. Peas and lentils are two of the best choices.
Vegetables and Fruits
When you’re going through cancer treatment, doctors advise filling up at least half of your plate with vegetables and fruits. Leafy green vegetables are a particularly good choice, since they’re rich in vitamins A, E, and K. They also contain a lot of iron, to keep your blood healthy. Cruciferous vegetables, like broccoli and cauliflower, contain antioxidant compounds that may stop cancer cells from growing. In one study by the National Cancer Institute, eating one to two cups of cruciferous vegetables a day caused participants to experience a 22 percent decrease in oxidative cellular damage caused by free radicals. Get more vegetables and fruits in your diet by snacking on them during the day.
Good nutrition is a vital part of cancer treatment, since it can help your body stay strong. The right foods may even fight the cancer itself. The better you’re able to eat, the more strength and energy you’ll have to draw from throughout the course of your treatment.
More
A New Study Says U.S. Lung Cancer Rates Are Falling
 Lung cancers are the most dangerous cancers in the United States, but according to recent data from the National Cancer Institute, there’s good news — rates of lung cancer in America are falling. That may be because of increased awareness of the dangers of smoking, and increase prevalence of smoke-free public spaces. While experts have already known that lung cancer rates in America have been dropping off, this latest study gives exact figures, and information about trends in the rates of various subtypes of lung cancer. The overall number of lung cancer cases declined by 12 percent between 1977 and 2010, researchers report.
Lung cancers are the most dangerous cancers in the United States, but according to recent data from the National Cancer Institute, there’s good news — rates of lung cancer in America are falling. That may be because of increased awareness of the dangers of smoking, and increase prevalence of smoke-free public spaces. While experts have already known that lung cancer rates in America have been dropping off, this latest study gives exact figures, and information about trends in the rates of various subtypes of lung cancer. The overall number of lung cancer cases declined by 12 percent between 1977 and 2010, researchers report.
Some Subtypes of Lung Cancer on the Decline
In this latest study, National Cancer Institute researcher Dr. Denise Lewis and her team analyzed data collected from over 450,000 people diagnosed with some type of lung cancer between 1977 and 2010. The data were collected as part of the Surveillance, Epidemiology, and End Results (SEER) Program.
The researchers wanted to learn more about the rates of specific lung cancer subtypes among various ethnicities and among men as compared to women. They looked at lung cancer rates among whites, blacks, non-white Hispanics, Asians and Pacific Islanders, and white Hispanics diagnosed between 1992 and 2010. Dr. Lewis and colleagues discovered that rates of small cell and squamous cell carcinomas have dropped off significantly since the 1990s. The researchers also discovered a decline in the overall number of non-specified lung-cancer cases.
Rates of these cancers among men have dropped off much more than they have among women. It’s believed that’s because men start smoking at a younger age than women, and so begin to develop lung cancer much sooner. With time, the researchers expect male and female lung cancer rates to approach one another.
While the rates of certain lung cancers are on the decline, there’s bad news, too. Rates of at least one lung cancer subtype are increasing.
 Adenocarcinomas on the Rise
Adenocarcinomas on the Rise
Rates of adenocarcinoma, a slow-growing subtype of lung cancer that appears in the outer layers of the lung tissue, are increasing. Dr. Normal Edelman of the American Lung Association believes that recent changes in the way people use cigarettes are to blame for increasing adenocarcinoma rates. In recent decades, low-nicotine, low-tar cigarettes have become more popular. People who smoke these cigarettes are more likely to smoke more and inhale the smoke more deeply, in an effort to get more nicotine out of them.
“The deeper you breathe in smoke, the more likely the cancer-causing tars are going to get into the outer area of the lungs, and that’s where adenocarcinoma starts,” Dr. Edelman told WebMD.
But since adenocarcinoma is a slower-growing form of lung cancer, it’s more likely than some subtypes to be diagnosed before it spreads outside the lungs. This means that lung cancer treatments for adenocarcinoma are more likely to be effective.
Cigarette smoking is still directly responsible for 90 to 95 percent of lung cancer cases diagnosed in the United States. It has even been called a contributing factor in cases where other carcinogens, like radon, were involved. As smoking becomes less and less common, researchers believe that lung cancer, too, will become rare.
More
5 Pancreatic Cancer Myths, Busted
 Pancreatic cancer has a bad reputation. It’s known for being one of the most difficult cancers to treat, in part because its early symptoms can be so difficult to pinpoint. Symptoms like jaundice, loss of appetite, abdominal pain, weight loss and general weakness can be indicative of a range of health problems — they aren’t necessarily pancreatic cancer. Plus, there’s no basic diagnostic test that can help physicians screen for pancreatic cancer. Myths about this scary form of cancer abound, but it’s important that you have the facts about pancreatic cancer if you want to defeat it.
Pancreatic cancer has a bad reputation. It’s known for being one of the most difficult cancers to treat, in part because its early symptoms can be so difficult to pinpoint. Symptoms like jaundice, loss of appetite, abdominal pain, weight loss and general weakness can be indicative of a range of health problems — they aren’t necessarily pancreatic cancer. Plus, there’s no basic diagnostic test that can help physicians screen for pancreatic cancer. Myths about this scary form of cancer abound, but it’s important that you have the facts about pancreatic cancer if you want to defeat it.
Myth 1: Pancreatic Cancer Is Always Deadly
Let’s get this damaging myth out of the way first. Pancreatic cancer is not always deadly — far from it. Like other forms of cancer, early detection is the key to successful treatment. Five-year survival rates are highest among those who are diagnosed early, and advances in pancreatic cancer treatment have made the disease much more survivable than it has been in the past. If you’re worried about developing pancreatic cancer, don’t be — it’s a relatively rare form of cancer, occurring in about 30,000 people a year. Just five to ten percent of cases are hereditary.
Myth 2: Pancreatic Cancer Screening Tests Are Available and Common
Unfortunately, pancreatic cancer screening tests are not commonly done. In fact, researchers have not yet developed an easy and accurate way to screen for pancreatic cancer. Unlike prostate or breast cancers, for example, there’s no blood test or specific imaging procedure that can reliably detect this cancer. CT scans can detect prostate tumors, but only a biopsy can determine if those tumors are cancerous.
Myth 3: There Is Only One Kind of Prostate Cancer
There are actually two kinds of pancreatic cancer. The vast majority — 95 percent — of pancreatic cancers are of a type known as adenocarcinoma. These tumors arise in the ductal cells that line the pancreatic ducts. The other, rarer form of pancreatic cancer occurs in the islets of Langerhans, the cells of the pancreas itself, where insulin is made. Cancer in these cells is known as islet-cell pancreatic cancer.
Myth 4: You Should Avoid Physical Contact with Others During Radiation Therapy
 This myth arose out of an understandable concern that radiation treatment could actually make a patient radioactive, placing his or her friends and loved ones at risk. However, the radiation used to treat pancreatic cancer doesn’t hang around in the body.
This myth arose out of an understandable concern that radiation treatment could actually make a patient radioactive, placing his or her friends and loved ones at risk. However, the radiation used to treat pancreatic cancer doesn’t hang around in the body.
Once you have finished a treatment session, you can feel free to go home and hug your loved ones at will. They are not at risk of being exposed to radiation because you are going through treatment. Physical contact with loved ones can be beneficial for all of you.
Myth 5: Surgery Makes Pancreatic Cancer More Likely to Spread
Lots of people know somebody who received surgery for pancreatic cancer, or another type of cancer, only to find that their cancer metastasized after surgery. However, it’s a myth that surgery for pancreatic cancer can cause it to spread by exposing the cancer to the air or lowering immunity. Surgery can’t cause cancer to spread, but it can prevent it from spreading.
The more you know about pancreatic cancer, the better your chances of recovering from it. With early detection and the right treatment plan, you can put pancreatic cancer behind you — where it belongs.
More
Study Links Vasectomy to Prostate Cancer
 A new study from the Harvard School of Public Health (HSPH) has found that men who have vasectomies are at an increased risk of developing prostate cancer. The researchers found no significant increase in the risk of low-grade prostate cancer among men with vasectomies, but instead found that those who had undergone the sterilization procedure had a higher risk of advanced and lethal prostate cancer. Overall, men who had vasectomies had about a 10 percent higher risk of prostate cancer than those who had not.
A new study from the Harvard School of Public Health (HSPH) has found that men who have vasectomies are at an increased risk of developing prostate cancer. The researchers found no significant increase in the risk of low-grade prostate cancer among men with vasectomies, but instead found that those who had undergone the sterilization procedure had a higher risk of advanced and lethal prostate cancer. Overall, men who had vasectomies had about a 10 percent higher risk of prostate cancer than those who had not.
Largest Ever Study into Vasectomy/Prostate Cancer Link
The HSPH study, which appeared online in the Journal of Clinical Oncology on July 7, 2012, is the most comprehensive such study to look at the link between vasectomy and prostate cancer risk. It was a follow-up to HSPH’s 1993 study on vasectomy and prostate cancer risk. The researchers followed 49,405 men for 24 years, from 1986 to 2010. Twenty-five percent of the men in the study had had a vasectomy.
Over the course of the study period, 6,023 men were diagnosed with prostate cancer. 811 of those died of prostate cancer. The researchers found that a previous vasectomy was associated with a 20 percent higher risk of advanced prostate cancer and a 19 percent higher risk of lethal prostate cancer. Among men who received regular PSA screenings, the relative increase in lethal prostate cancer risk was 56 percent.
The researchers found that the younger a man was at the time of his vasectomy, the greater his risk for advanced or lethal prostate cancer. Men who had had their vasectomies before 38 years of age were found to be at the highest risk.
Researchers Rule out Bias
Previous studies into the possibility of a link between vasectomy and prostate cancer may have been biased. For one thing, men who receive vasectomies tend to receive better medical care and more regular PSA screening, meaning that they’d be more likely than men who did not receive vasectomies to be diagnosed with prostate cancer.
Nor could previous studies rule out the possibility that sexually transmitted infections or other potential risk factors may have contributed to higher rates of prostate cancer among study participants. For this study, however, researchers had access to enough information about the study participants to rule out these potential biases.
Overall Increase in Risk Is Small
 If you’re one of the 15 percent of American men who have had a vasectomy, don’t panic yet. The overall increase in prostate cancer risk for men who have had vasectomies is small — just 10 percent.
If you’re one of the 15 percent of American men who have had a vasectomy, don’t panic yet. The overall increase in prostate cancer risk for men who have had vasectomies is small — just 10 percent.
Since previous research has failed to find a clear-cut link between vasectomy and prostate cancer, many experts advise taking these findings with a grain of salt. Prostate cancer treatments are steadily improving, and most men diagnosed with the disease don’t die from it.
Dr. Louis Kavoussi, chairman of urology at North Shore-LIJ Health System in New Hyde Park, N.Y., told CBS News, “I would be cautious about applying these findings to clinical practice right now. This is not like cigarette smoking causing a large number of people to develop lung cancer. This is a small increase in the risk of prostate cancer.”
New data from a HSPH study found a link between vasectomy and prostate cancer. Men who have had vasectomies are 10 percent more likely to develop prostate cancer. If you have had a vasectomy, don’t let it keep you up at night — experts say the relative increased risk is small.
More
 A cancer diagnosis can be one of the most overwhelming to receive, and if you’re like many patients, you may feel rushed to make decisions about your treatment. While your doctor may want you to start looking at treatment options as soon as you receive your diagnosis, you’ll most likely have some time to think things over and decide for yourself what treatment plan will work best for you. Remember that your ultimate decision doesn’t have to be set in stone — if you change your mind about treatment midway through the process, that’s okay, too.
A cancer diagnosis can be one of the most overwhelming to receive, and if you’re like many patients, you may feel rushed to make decisions about your treatment. While your doctor may want you to start looking at treatment options as soon as you receive your diagnosis, you’ll most likely have some time to think things over and decide for yourself what treatment plan will work best for you. Remember that your ultimate decision doesn’t have to be set in stone — if you change your mind about treatment midway through the process, that’s okay, too. If side effects are too severe or you have second thoughts about your treatment decision, you’re allowed to change your mind. Treatment can affect your health, career, and personal life in ways you might not expect. It’s part of your treatment team’s job to help you cope with these changes.
If side effects are too severe or you have second thoughts about your treatment decision, you’re allowed to change your mind. Treatment can affect your health, career, and personal life in ways you might not expect. It’s part of your treatment team’s job to help you cope with these changes.



 Adenocarcinomas on the Rise
Adenocarcinomas on the Rise


